As is true with many things in life, there may be more contributing to your pain than meets the eye. In fact, the point of pain may not be the source. Muscles throughout the body can create myofascial trigger points, often referred to as “knots.” These palpable tender spots are a group of muscle fibers that maintain a semi-contracted state for too long. The fascia, which is a non- contractile tissue, covers nearly every muscle fiber, can also be a part of this point restriction. These restrictions can be very tender to touch and can have a greater influence on how the entire muscle activates. Through years of research, medical professionals have been able to map common referral patterns for each muscle1.
What is Dry Needling?
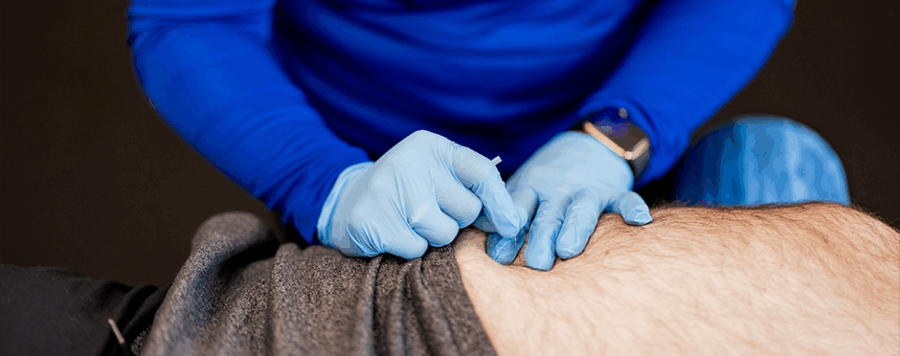
Dry needling is a technique that uses a thin monofilament needle into the trigger point. Upon insertion into the trigger point, there is often an associated muscle twitch. This twitch causes a reflex allowing for the restricted area to relax. This relaxation addresses the referred pain and improves global muscle activation.
These trigger points can be overlooked when trying to diagnosis painful symptoms. Three common pain patterns that may benefit from dry needling as a treatment include the following.
1. Headaches
There are many muscles around the neck and shoulders that have referral patterns to the head and face. These referral patterns may mimic tension headaches that seem to begin at the base of the skull and move upward. There are also muscles that may recreate headaches along the forehead or at the temples.
Sinus pressure or sinus headaches may be coming from a muscle along the front of your neck. This muscle can be responsible for sinus pressure or headaches that seem to arch around your eye socket.
If trigger points are the source of referred pain causing headaches, dry needling can be an efficient way of relieving pain. With decreased muscle tension along with exercises and manual techniques to improve cervical spine mobility, the effects of dry needling may be sustained.
2. Carpal Tunnel
Carpal tunnel is often identified by the numbness and tingling in the hands. True carpal tunnel syndrome is caused by increased pressure along the median nerve as it crosses the wrist. However, there are several muscles in the shoulder girdle that can mimic numbness, tingling, or pain in the wrist, hand, or fingers.
Dry needling can be a good option to help resolve unequal tension along muscles that cross the wrist as well as addressing trigger points that may be referring to the wrist or hand. With improved muscle tension, length and trigger point release, supportive strengthening exercises may be more effective. Proper forearm support and ensuring your wrists are in a neutral position while working at a computer can help prolong the positive effects of dry needling and exercises.
3. Plantar Fasciitis
The muscles in your calves, particularly the gastrocnemius and soleus, can cause pain to travel to the heel and arch of your foot. These muscles can also be closely related to increased tension along the fascia in your foot. While adjunct strengthening, stretching, and ice may benefit plantar fasciitis pain, addressing trigger points higher up in the leg may provide more complete care for this common diagnosis.
A common question that is often associated with dry needling is, does it hurt? There is often a discomfort from achieving the muscle twitch. The needle is so thin and typically the insertion is not painful. The muscle twitch often feels like deep pressure or similar to a muscle cramp. There may be lingering soreness following treatment, but gentle stretching and heating pads often address this after effect.
A great aspect about dry needling is that, if the trigger point is part of causing symptoms, relief may be felt shortly after needling. Dry needling is most beneficial when used in adjunct with prescribed strengthening exercises to address the source of muscle imbalances. An Athletico physical therapist can get you started with dry needling to help relive any pain you may be experiencing.
Find a Dry Needling Therapist Near You
References:
1. Shah, Jay P., Nikki Thaker, Juliana Heimur, Jacqueline V. Aredo, Siddhartha Sikdar, and Lynn Gerber. “Myofascial Trigger Points Then and Now: A Historical and Scientific Perspective.” PM&R 7, no. 7 (2015): 746–61. https://doi.org/10.1016/j.pmrj.2015.01.024.

 width="900"
height="356"
>
width="900"
height="356"
>

1 Comment
Judy Thomas
Looking for a pt Dr. that does myofacial Treatment for my chronic neck pain for 40 +years