History of BFR
In 1966, 18-year-old Yoshiaki Sato had an epiphany after standing up from a “seiza” position at a funeral – his legs felt as if they had been through a fatiguing workout. After a catastrophic ankle injury skiing in 1973, he was in a long leg cast for six weeks. During his immobilization, Sato initiated the first “blood flow restriction training” by using belts and performing isometric exercises. Doctors were shocked when his leg was not atrophied or tender when the cast was removed. Throughout the 1970s, Sato investigated restriction training on himself and other Japanese body builders. During the 1980s, Sato started his own personal training clinic, introducing “occlusion training,” quickly catching on with European body builders as well. In the 1990s, Sato started doing formal research and developed “KAATSU” pneumatic bands. “Ka” means “additional” and “Atsu” means “pressure.” Use of Sato’s formal KAATSU equipment requires formal apprenticeship in Japan, so many Westerners have made use of various wraps, straps, bands, belts, blood pressure cuffs and surgical tourniquets in attempt to replicate Dr. Sato’s results.
BFR rehabilitation has gained more wide-spread popularity as it started being used for military personnel who were struggling to improve muscle strength and size in their injured limbs after blast injuries, amputations and limb salvage procedures. When attempting to lift heavy weights, they were significantly limited due to pain and weakness. With the help of BFR training, they were able to achieve their strengthening goals using lighter weights. Olympic athletes have since caught on to BFR taking workouts to the point of fatigue without the heavy lifting. Now BFR is becoming more popular in outpatient physical therapy as well, as it can help minimize the effects of limited extremity use.
What is BFR?
During BFR training, a patient or athlete works out with a narrow, elastic band around the upper portions of the exercising arm or leg. This band partially restricts venous blood flow but does not affect arterial inflow to the extremity. Doing this produces a systemic response comparative to heavy weight training. Performing high repetitions of a particular exercise while wearing the elastic band and using light weights will allow the patient to receive the strengthening benefits of heavy lifting without the stress to tissues that may be healing from a recent injury or surgery.
How Does This Work?
In a nutshell, exercising with lighter weights while using blood flow restriction causes a local disturbance of homeostasis, as the working muscle does not receive enough blood flow to sustain contractions. This creates a release of autonomic and anabolic hormones that move throughout the body. This systemic response augments the local response, causing increased protein synthesis. Because little damage is done to the soft tissue by avoiding heavy weight lifting, improvements in strength and endurance can come quickly. All tissues both proximal and distal to the blood flow restriction bands can benefit from these effects.
Who Benefits from BFR?
 BFR training can be performed in a regular fitness routine, but can also be safely performed under the supervision of trained professionals in outpatient physical therapy clinics. BFR can safely be used on patients in the acute phase of rehabilitation following most upper or lower extremity surgeries, including ACL reconstruction, meniscectomy, hip/knee replacement, rotator cuff repair or any tendon repair. Research has shown BFR can minimize loss of muscle mass and decrease bony healing time during the early immobilization phases, allowing patients to improve both muscle size and strength without the stress of heavy lifting on healing soft tissue. Patients with osteoarthritis, rheumatoid arthritis, osteopenia or osteoporosis may also benefit from BFR. Additionally, BFR has been utilized after strokes or spinal cord injuries and with athletes who want to improve performance.
BFR training can be performed in a regular fitness routine, but can also be safely performed under the supervision of trained professionals in outpatient physical therapy clinics. BFR can safely be used on patients in the acute phase of rehabilitation following most upper or lower extremity surgeries, including ACL reconstruction, meniscectomy, hip/knee replacement, rotator cuff repair or any tendon repair. Research has shown BFR can minimize loss of muscle mass and decrease bony healing time during the early immobilization phases, allowing patients to improve both muscle size and strength without the stress of heavy lifting on healing soft tissue. Patients with osteoarthritis, rheumatoid arthritis, osteopenia or osteoporosis may also benefit from BFR. Additionally, BFR has been utilized after strokes or spinal cord injuries and with athletes who want to improve performance.
Is BFR Safe?
Research has shown that BFR is not only comfortable for the patient, but also safe and effective when exercises are performed appropriately and when equipment is monitored by a trained blood flow restriction professional. This service is now available to be performed by trained clinicians at select Athletico clinics. If you are interested in learning more about BFR, click the button below to request an appointment.
The Athletico blog is an educational resource written by Athletico employees. Athletico bloggers are licensed professionals who abide by the code of ethics outlined by their respective professional associations. The content published in blog posts represents the opinion of the individual author based on their expertise and experience. The content provided in this blog is for informational purposes only, does not constitute medical advice and should not be relied on for making personal health decisions.
References
Dankel, S., Jessee, M., Abe, T., & Loenneke, J. (2016). The effects of blood flow restriction on
upper-body musculature located distal and proximal to applied pressure. Sports Medicine,
46(1), 23-33. doi:10.1007/s40279-015-0407-7
Loenneke, J. P., Thiebaud, R. S., & Abe, T. (2014). Does blood flow restriction result in skeletal
muscle damage? A critical review of available evidence. Scandinavian Journal of
Medicine & Science in Sports, 24(6), e415-422.
Nakajima et al. (2006). Use and safety of KAATSU training: Results of a national survey. International Journal of KAATSU Training Research, 2(1):5-13.
Segal, N.A., Williams, G.N., Davis, M., Wallace, R.B., & Mikesky, A. (2015). Efficacy of blood
flow restricted low-load resistance training in women with risk factors for symptomatic knee osteoarthritis. PM & R: Journal of Injury, Function & Rehabilitation, 7(4), 376-384.
doi: 10.1016/j.pmrj.2014.09.014
Slysz, J., Stultz, J., & Burr, J.F. (2015). The efficacy of blood flow restricted exercise: A systematic
review & meta-analysis. Journal of Science & Medicine in Sport / Sports Medicine
Australia. Doi:10.1016/j.jsams.2015.09.005
Takarada et al (2000). Effects of resistance exercise combined with moderate vascular occlusion on muscular function in humans. J. Appl. Physiology 88: 2097-2106, 2000

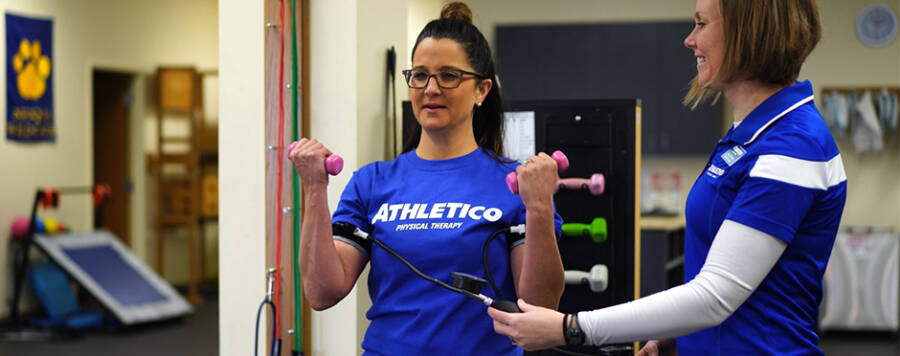 width="900"
height="356"
>
width="900"
height="356"
>

12 Comments
Mallory Hansen
I am currently a student physical therapist and doing an in-service on BFRT. I am wondering how you bill for BFRT during PT sessions? I can’t seem to find anything about how PT’s can bill for this.
Don
It would likely be billed under Therx or vasopneumatic device
Lori Frymier
It feels like they are stabbing a knife into my thigh when they are using it. What do you mean by it being monitored by a trained professional, they just turn it on and walk away? I am over 60 and don’t feel well for hours after the treatment. I have a knee problem.
Athletico
Lori – Please let your physical therapist know about your symptoms so they can adjust pressure, modify the exercise being performed with BFR, or alter your treatment plan. BFR should cause soreness and fatigue but definitely not sharp pain.
Sam
The Wisconsin state practice act is silent on whether PTs are able to perform this intervention. Is there anything written showing that PTs are able to perform this specifically in the state of Wisconsin?
Athletico
Thank you for your comment. For questions related to clinical practice in the state of Wisconsin, you can contact the Wisconsin Department of Safety and Professional Services.
Marsha Parise
The next day after PT using the BFR method, I could barely walk. My knee swelled to the size of a cantaloup. I’m a 58 yr old female in great physical shape, post ACL reconstruction. This first therapy session was on a thursday, so my next appointment was to be the upcoming tuesday. My therapist said not to do any home exercises. I’m confused because I had a totally different protocol 5 yrs ago when my other knee also had ACL reconstruction.
Athletico
Hi Marsha – Please call your physical therapist before your next appointment to discuss your response to BFR. Soreness and fatigue are desired responses, but significant swelling and difficulty walking are not appropriate responses. There are many different kinds of BFR (some narrow elastic bands vs other tourniquet devices), so without knowing which kind you had done, it is hard to make recommendations for adjusting BFR next treatment vs. avoiding it. Please also ask more questions of your PT around the home exercise program and the possibility of doing appropriate exercises at home to help meet your early post-op goals.
Rich
I’ve been using the BFR for weeks and it is really incredible in speeding up my body helping build muscle in quad and leg after old ACL injuries.
I have chronic pain from old injuries and bone trauma, so there is atrophy and dysfunction of the left leg.
My doctors all just say I need PT, which honestly I neglected through the years.
This BFR technique has really helped me show gains.
I will say though that I am claustrophobic, and when that thing is firing and I am laying on my back doing quad sets / leg raises, I get really kinda anxious… but I make sure I get through the 8 minutes.
However, my standing exercises with the machine firing… shallow squats, calf raises, lunges … I don’t have that anxious or claustrophobic feeling.
This is the second 6 week PT regimen I am doing over the last year, both times, I look forward to pushing my body with the BFR, because I am seeing results!
Please feel free to fire off any questions to me.
Athletico
Hello Rich, we’re so glad to hear Blood Flow Restriction is helping you!
Mike
I’m looking for resources to help me find the proper “fit” and pressure for my legs and arms. I’ve learned to find the max pressure (total BF occlusion) by using a Doppler to hear when my pulse stops at my foot. Then back off the pressure to 80% or 50%. Is there a way to find this range without a pedal pulse?
Athletico
Mike – Every brand of BFR is different, and we recommend that you follow the manufacturer’s guidelines. The brand that Athletico has partnered with uses a narrow elastic band that cannot completely occlude arterial inflow even if pumped all the way up to 500 mmHg. This brand has various recommended starting pressures based on band size and limb. Other wide, rigid tourniquet cuff brands that are designed to occlude go off limb occlusion pressure, which requires a doppler and pulses.